Insight
How Leading Health Systems Are Closing the Access Execution Gap
What health system leaders shared in a recent Tegria and THMA webinar
Health systems across the country are investing heavily in improving patient access. Yet for many organizations, turning strategy into consistent, measurable results remains a familiar, persistent challenge.
On March 25, 2026, Tegria partnered with The Health Management Academy (THMA) to host a virtual panel, “Beyond the Digital Front Door: Building an Access-Driven Enterprise.” The discussion brought together leaders from Emory Healthcare, Sutter Health, and Indiana University Health to explore how they are addressing one of the industry’s most pressing issues—closing the gap between access strategy and execution.
The conversation reinforced a key finding from the Access-Driven Enterprise (ADE) research. While access is now widely recognized as a strategic priority, many organizations continue to face challenges related to governance, operational alignment, and return on investment.
What stood out in this session was not just the persistence of these challenges, but the different ways leading systems are working to overcome them.
Emory Healthcare: From Rapid Improvement to Long-Term Discipline
Alignment needs to be applied in practice. Monthly executive check-ins, shared accountability, public commitment, I think, really helped us turn executive prioritization into actual execution.
HALEY BOLTONVP, Access Performance Management at Emory Healthcare
At Emory Healthcare, the journey began with a sense of urgency. Leaders recognized that improving access required immediate action, particularly as demand increased and expectations evolved. They launched a focused, systemwide effort to expand appointment availability and improve timeliness of care.
This initial push helped create momentum across the organization. Teams revisited scheduling practices, identified new ways to open capacity, and began aligning around shared goals. The effort demonstrated that meaningful improvement was possible, even within complex operational environments.
At the same time, leaders recognized that urgency alone would not sustain progress. Maintaining gains required a more structured approach, supported by consistent governance and clearer accountability. Emory shifted its focus toward building a stronger operational foundation, including more standardized reporting and closer collaboration across clinical, operational, and administrative teams.
That evolution reflects a broader lesson: Rapid improvement can spark change, but lasting impact depends on discipline, infrastructure, and ongoing alignment.
Sutter Health: Letting Digital Access Lead the Way
Access is a strategic decision, not a technical one. The technology exists to do this well. It’s really, culturally, are we willing to put consumers first and make bold choices to give them an experience like they get in so many other aspects of their life?
ANDREW SMITHVP, Access, Sutter Health
Sutter Health took a different approach by using digital access as a catalyst for transformation. Rather than waiting to optimize workflows before expanding access, leaders made a deliberate decision to scale online scheduling across the organization and align teams around that goal.
This decision created immediate pressure to address underlying challenges. Supporting digital scheduling required more consistent templates, clearer referral pathways, and better coordination across a decentralized network of providers. What began as a digital initiative quickly became an enterprise-wide effort to standardize and streamline operations.
As those changes took hold, adoption of online scheduling increased significantly, reflecting both improved access and stronger alignment between technology and workflows.
Beyond operational improvements, Sutter’s experience highlights how access can influence broader organizational outcomes. Reducing friction in how patients enter the system can strengthen engagement and support long-term growth.
Indiana University Health: Looking Beyond the Front Door
If you just turn on the technology, but nobody can find an appointment slot, have you actually made a net improvement?
JEREMY ROGERSVP, Digital Access and Experience, Indiana University Health
IU Health focused on a different dimension of the access challenge by expanding its view beyond the initial point of entry. Leaders observed that improving the first appointment experience was only part of the equation. Patients often encountered delays and friction later in their journey, particularly when navigating referrals, diagnostics, or follow-up care. These breakdowns could undermine the overall experience, even when front-end access had improved.
In response, IU Health emphasized a more holistic approach. Efforts centered on better coordination across the care continuum, supported by more consistent data and workflows. Leaders also worked to balance standardization with the realities of different specialties, recognizing that a single approach would not meet every need.
This perspective reflects an important shift. Access is not just about getting patients in the door. It is about ensuring they can move through the system efficiently and receive timely, coordinated care.
A Common Thread: Access as an Enterprise Capability
While each organization approached the challenge differently, several common themes emerged.
- First, access challenges are rarely solved through technology alone. Most health systems already have digital tools in place. The more complex work involves aligning people, processes, and priorities across the organization.
- Second, progress requires both speed and structure. Focused initiatives can help drive early gains, but sustained improvement depends on governance, standardization, and clear accountability.
- Finally, access must be treated as an enterprise capability. It touches every part of the organization, from scheduling and staffing to clinical operations and financial performance. Improvements in one area often depend on changes in another, making cross-functional alignment essential.
Health systems that recognize this broader scope are better positioned to close execution gaps and realize the full value of their access strategies.
Watch the Webinar and Explore the Full Research
The approaches highlighted here represent just a snapshot of how leading organizations are addressing access challenges.
To hear directly from these leaders and explore the full findings, download The Access-Driven Enterprise report and watch the full webinar recording. Together, they offer deeper insight into how health systems are aligning strategy, operations, and investment to improve access at scale.
Insight
From Strategy to Execution: Key Insights From HIMSS26
Each year, the HIMSS Global Health Conference & Exhibition brings together healthcare leaders, innovators, and policymakers to explore the technologies and strategies shaping the future of healthcare. HIMSS26, held March 9–12 in Las Vegas, convened thousands of industry stakeholders to discuss the evolving role of AI, digital transformation, and operational strategy in a rapidly changing healthcare landscape.
Across the conference, one theme surfaced repeatedly: Successful transformation depends on strong alignment between strategy, operations, and technology. Whether the conversation focused on patient access, revenue cycle performance, or large-scale technology adoption, healthcare leaders emphasized the importance of connecting strategy, operations, and technology to deliver measurable outcomes.
Tegria contributed to these conversations through three sessions exploring how healthcare organizations can bridge the gap between strategic priorities and operational execution. From improving patient access to strengthening change management and preventing revenue cycle denials, the discussions highlighted practical strategies health systems are using to navigate today’s challenges while preparing for the future.
Closing the Access Execution Gap

Tegria’s HIMSS26 programming began on Tuesday with “How Leading Health Systems Are Closing the Access Execution Gap,” presented by Steve Nilson, Acting Director of Access & Experience at Tegria, and Wes Adams, Senior Director at The Health Management Academy (THMA). The session shared original research conducted jointly by Tegria and THMA examining how health systems are defining and operationalizing patient access strategy.
Drawing on surveys and executive interviews with health system leaders conducted in late 2025, Nilson and Adams explained that patient access has rapidly evolved from an operational metric into a strategic priority. The research found that 82% of health systems now identify access as a strategic pillar, placing it alongside growth, quality, and financial performance as a key driver of enterprise success. Yet many organizations struggle to translate strategy into results. Nilson and Adams described persistent gaps in governance, ROI measurement, and operational execution, emphasizing that closing these gaps requires stronger alignment between leadership, operations, and technology teams.
82% of health systems say patient access is now a strategic pillar—but many still struggle to operationalize it.
Don’t Gamble on ROI: Win Big With Change Management

On Wednesday, Meg Johnson, Director of Care Operations at Tegria, joined Robbie Bullough, Senior Director of Consulting at KLAS Research, to present “Don’t Gamble on ROI: Win Big With Change Management.” The session explored one of the most persistent barriers to healthcare transformation: the difficulty organizations face in achieving adoption and measurable results from new technology investments.
Johnson and Bullough explained that, while health systems often focus on selecting the right technology, the real determinant of success is how effectively organizations manage the human and operational aspects of change. Drawing on insights from KLAS Research, the speakers shared how organizations that prioritize structured change management are significantly more likely to realize the value of their technology investments. They also introduced the KLAS Change Management Framework, which helps organizations engage stakeholders early, align operational teams, and establish clear adoption metrics that extend beyond go-live.
Organizations that prioritize change management are seven times more likely to achieve successful outcomes from technology initiatives.
Denied No More: A Revenue Recovery Playbook

Later that day, Jay Nelson, Principal at Tegria, joined Michael Newsome, Director at Novant Health, to present “Denied No More: A Revenue Recovery Playbook.” The session focused on strategies health systems can use to identify and prevent bundled denials, an often overlooked but significant contributor to revenue loss.
Nelson and Newsome discussed how many bundled denials stem from evolving payer policies, coding conflicts, and inconsistencies in billing rules that can be difficult to detect without deeper revenue cycle analytics. By analyzing denial patterns and implementing stronger front-end edits, organizations can prevent many of these issues before claims are submitted. The presenters also highlighted the role of cross-functional collaboration between clinical, coding, and revenue cycle teams, along with emerging AI-driven tools that help organizations anticipate policy changes and identify denial risks earlier. Through these strategies, Novant Health has achieved a 99.88% clean claim rate through its clearinghouse, demonstrating how proactive analytics and operational coordination can significantly reduce preventable denials.
Novant Health achieved a 99.88% clean claim rate through proactive denial prevention strategies.
Looking Ahead
The conversations at HIMSS26 reinforced a reality healthcare leaders know well: Technology transformation is as much about organizational alignment as it is about innovation. As health systems navigate growing financial pressures, workforce challenges, and rapidly evolving technologies, success will increasingly depend on their ability to connect strategy, operations, and data-driven decision-making.
For Tegria, HIMSS continues to be an important forum for sharing insights and learning from healthcare leaders across the industry. The discussions in Las Vegas underscored the importance of practical, operationally grounded strategies for all aspects of care, from improving patient access and strengthening revenue cycle performance to ensuring that technology investments deliver meaningful results.
We look forward to continuing these conversations with healthcare organizations working to turn strategy into sustainable transformation.
2026 Industry Research
Access Is a Strategic Pillar.
Is Your Execution Keeping Up?

Access has entered a new strategic era.
Access is no longer about getting an appointment. New research from Tegria and The Health Management Academy reveals how health systems are redefining access as an enterprise capability—the investments they’re making, the execution gaps they’re facing, and the barriers standing in their way. Discover what’s driving transformation and where opportunities lie.
Investment vs. Results
“While organizations have invested heavily in their digital ecosystems, few have yet realized the seamless experience patients expect.”
THE ACCESS-DRIVEN ENTERPRISE REPORT
Big Goals, Constrained Resources
Leaders are focused on driving patient experience, but funding and ROI expectations are misaligned.

Strategic Intent
Health systems are taking diverse steps to improve access across multiple domains, investing in digital tools, advancing AI, and improving point-of-care experiences.
Top Access Investments
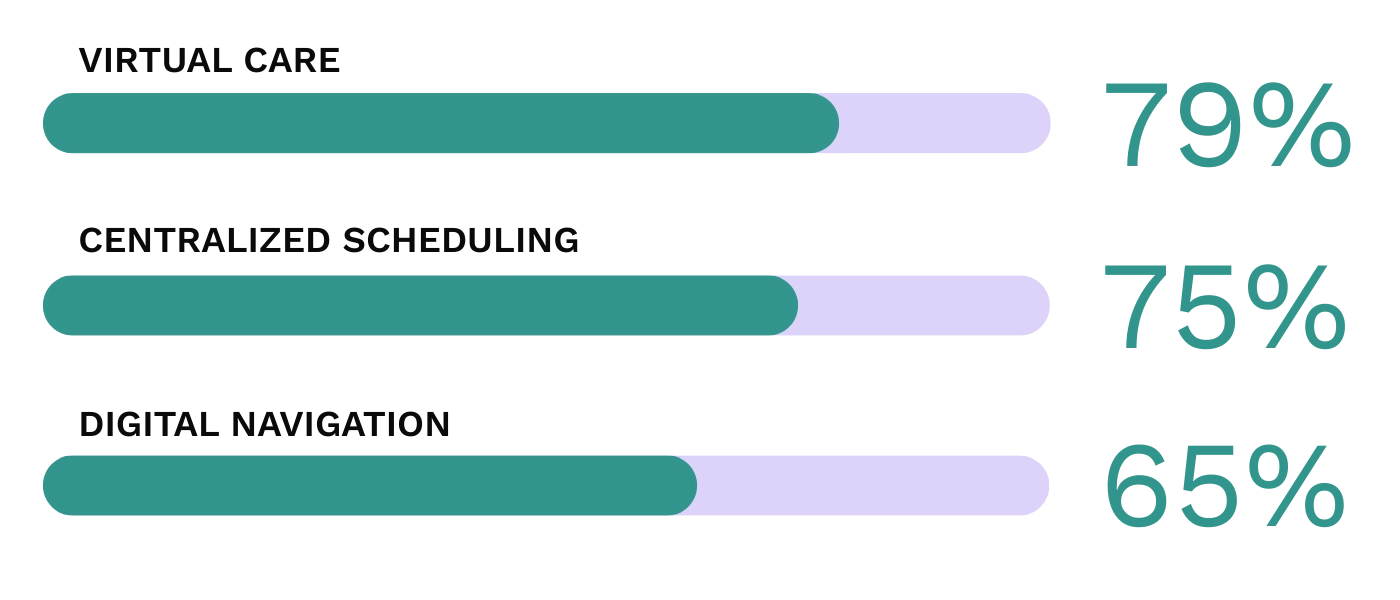
Top Barriers to Success

Execution Reality
Health systems continue to struggle translating ambition into execution. These are the areas where leaders are reporting the largest gaps between access goals and current capabilities.
The Path Forward
Health systems are dedicated to improving access, with 93% reviewing access strategy at least quarterly. The report outlines key strategies to help systems bridge the access execution gap.
Download the Full Research Report
Benchmark your access strategy against peers
Spot execution gaps that stall ROI
See where leading systems are investing
Close the strategy-to-execution gap

Insight
Making Digital Health Work: What’s Next for Patient Access
The Next Chapter in Access-Driven Care
Digital tools are now a routine part of how patients interact with the healthcare system. Per HIMSS, more than half of U.S. patients now use digital tools to communicate with their healthcare providers. From patient portals to online scheduling and virtual visits, technology has reshaped how people communicate with providers and manage aspects of their care. For many organizations, these tools represent years of investment and effort to modernize the patient experience.
And yet, for many patients, access still feels harder than it should.
Patients increasingly rely on digital tools to engage with their healthcare, but reliance does not always translate into confidence or clarity. Even as digital touchpoints multiply, many patients continue to experience fragmented journeys, uncertainty about next steps, and difficulty navigating care across providers and settings. These challenges often surface at moments when patients are already stressed or vulnerable, amplifying frustration rather than easing it.
Healthcare organizations have invested heavily in digital front doors. What is becoming increasingly clear is that digital progress, on its own, has not resolved the access challenge.
What the Industry Already Knows About Patient Expectations
A 2025 report from HIMSS reinforces a critical reality. Patients want digital experiences that feel supportive, complete, and designed with their needs in mind, not simply functional. Ease of use matters; but so do relevance, context, and continuity across interactions.
Insights from the KLAS Patient & Consumer Innovation Summit with patients and healthcare leaders point to a similar conclusion: Digital maturity has outpaced experience maturity, leaving many organizations with sophisticated tools but inconsistent access experiences.
Digital Tools Exist, but Patients Don’t Always Feel Considered
Patients consistently say partnership and engagement matter in their healthcare relationships. They want to feel informed, involved, and respected when interacting with digital systems, particularly as those systems increasingly mediate access to care.
Only about 41% of patients believe health systems consider patient needs when developing digital tools.
Source: HIMSS
This perception gap helps explain why access often feels disconnected. Tools may technically function as intended; but they do not always reflect how patients think, decide, or move through care. When patients feel that digital experiences were designed around internal workflows rather than patient needs, trust erodes quickly.
KLAS reinforces this point, highlighting that patients often struggle to understand who owns their next step or how different digital touchpoints fit together, particularly after visits or test results are delivered.
Incomplete Information Undermines Trust
Even when patients actively use portals and digital platforms, many report that the information they need is missing, delayed, or difficult to interpret. This lack of completeness undermines one of the core promises of digital health: clarity.
Only about 2 in 5 patients say their patient portal is never missing important health information.
Source: HIMSS
When information is incomplete or inconsistent, digital access can increase uncertainty rather than reduce it. Patients are left unsure whether they have the full picture, whether action is required, or where to turn next. In these moments, digital tools can unintentionally heighten anxiety instead of providing reassurance.
This uncertainty becomes especially pronounced when care involves multiple providers, referrals, or follow-up steps that span clinical and administrative boundaries.
The Access Gap: Why Digital Tools Alone Aren’t Enough
HIMSS findings suggest that the core issue is not whether patients are willing to engage digitally. It is whether digital experiences help patients feel informed, supported, and in control of their health decisions. That sense of control remains uneven across tools and use cases.
Only 57% of patients using wearable devices feel these tools give them control over their health.
Source: HIMSS
These numbers highlight a broader access gap. Digital tools may collect data or facilitate interaction, but they do not always help patients understand what that data means or how to act on it. Without clear guidance, data alone can feel overwhelming or irrelevant.
Research consistently points to similar frustrations: duplicative forms, unclear communication, difficulty reaching the right person, and confusion after visits or test results. Patients often receive messages across multiple channels without a clear sense of priority or direction, leaving them unsure of their role in the next step of care.
When access feels fragmented, patients don’t experience it as a digital problem. They experience it as uncertainty. True access is about helping patients understand where they are, what comes next, and how to move forward without friction.
STEVE NILSONPrincipal Program Manager, Access + Experience
Taken together, these challenges point to deeper issues that extend beyond interface design. They reflect gaps in workflow alignment, ownership, and coordination across the organization.
Five Early Moves To Prepare for Access Transformation
While no single change will resolve access challenges overnight, organizations preparing for the next phase of access transformation tend to focus on several early moves that reflect a broader shift in mindset. These moves signal readiness to think about access more holistically.
1. Simplify Intake and Navigation
Patients quickly lose confidence when they are asked to repeat information or navigate inconsistent workflows. Simplifying intake and reducing handoffs can ease friction for both patients and staff, while also improving data quality across systems.
2. Design for How Patients Actually Engage
Digital engagement is not one-size-fits-all. Patients move between digital, phone, and in-person channels depending on circumstance, comfort, and urgency. Per KLAS, access strategies that acknowledge this reality are better positioned to support continuity and reduce drop-off.
3. Embed Education Into Moments That Matter
Patients are most receptive to guidance during moments of uncertainty, such as receiving results, scheduling follow-ups, or transitioning between care settings. Delivering education at these moments helps patients feel supported rather than overwhelmed.
4. Use AI To Reduce Friction
HIMSS findings point to cautious optimism around AI when it is used to organize information, streamline communication, and support clinical understanding rather than overwhelm patients with additional complexity. Purposeful use matters more than novelty.
5. Treat Access as a Shared Responsibility
Access improves when digital, clinical, and operational teams align around common goals and shared accountability. Without that alignment, even well-designed tools struggle to deliver consistent experiences across the patient journey.
These moves are not a complete strategy. They are early indicators that organizations are preparing for a more coordinated approach to access.
The Next Chapter in Access-Driven Care
Digital health is not failing. It is unfinished.
As patient expectations rise and pressures related to capacity, workforce, and financial sustainability intensify, access can no longer be treated as a front-door function or a collection of disconnected tools. The next chapter requires coordination across people, process, data, and technology so digital investments translate into experiences that patients can understand, trust, and rely on over time.
Ready for Healthcare’s Next Step?
The Access-Driven Enterprise Report from Tegria and The Health Management Academy explores how leading healthcare organizations are making this shift, reframing access as a strategic capability that connects enterprise decision-making with real-world patient experience.
Insight
Boost Value-Based Care Performance in 2026
How To Bounce Back From Disappointing Results
Healthcare organizations can take control of their value-based care outcomes before results are finalized, not after. As 2025 value-based care performance comes into focus, many provider leaders are reassessing how results compared to expectations. While some organizations achieved strong shared savings and quality outcomes, others faced financial pressure, operational strain, or unexplained variation across populations and contracts. What made these outcomes particularly frustrating was that they often came as a surprise, even for organizations that believed they were well prepared. The result was performance that did not fully reflect the effort invested in value-based care initiatives.

Unexpected value-based care performance is increasingly common as organizations take on more risk and expand across multiple value-based payment models. These outcomes highlight how closely value-based success depends on operational execution, data-driven decision-making, and care delivery alignment. The organizations that improve fastest use performance surprises as a catalyst to invest in data analytics and interdisciplinary structures needed for value-based care success.
Building on our Succeeding in Value-Based Care series, this article outlines practical considerations and concrete steps VBC decision-makers can take to improve results in 2026.

What Drove Unexpected 2025 Value-Based Care Results?
When results don’t line up with forecasts, it rarely comes down to a single issue. Instead, organizations find that a familiar set of challenges surface in new and more visible ways as value-based care programs scale. These patterns can appear across data, operations, contracts, and workforce adoption.
- Data and analytics limitations remain a significant challenge. As VBC participation steadily grows, many organizations lack timely access to actionable cost, utilization, and quality insights. Delayed claims, inconsistent attribution, and fragmented data sources reduce visibility into performance drivers during the year.
- Care operations complexity also plays a central role. While many providers have invested in care coordination and population health strategies, execution varies across service lines, sites, and teams. Inconsistent workflows and limited standardization create performance variation that can be difficult to manage at scale.
- Risk contract dynamics further influence results. Shifts in utilization, benchmark recalculations, and changes in patient behavior affect financial outcomes in ways that were not always anticipated during contract modeling.
- Workforce adoption challenges compound these issues. Competing clinical priorities, staffing shortages, and workflow burden slow adoption of new tools and care processes designed to support value-based performance.
Together, these factors underscore the importance of operational readiness as a core capability for value-based care success.

Practical Steps To Strengthen Value-Based Care Performance
1. Improve Performance Visibility Through Integrated Data
Strong value-based care operations depend on integrated clinical, financial, and claims data that support ongoing performance management. Leaders need insight into attribution, utilization trends, care gaps, and cost drivers throughout the performance year.
Action step: Establish enterprise data governance and analytics workflows that align finance, care operations, and clinical leadership around shared performance metrics and dashboards.
2. Standardize and Scale Care Models
Organizations that achieved consistent results in 2025 focused on operationalizing care models beyond pilot programs. Standardized workflows, clearly defined roles, and measurable outcomes supported reliable execution across populations.
Action step: Translate care models into repeatable operational playbooks that embed risk-adjusted pathways into daily clinical and care management workflows.
3. Connect Care Delivery Decisions to Contract Incentives
Value-based contracts reward specific behaviors, workflows, and outcomes. Without ongoing alignment between care delivery and contract requirements, organizations may fall short of expected reimbursement despite significant effort.
Action step: Regularly assess how current care workflows and utilization patterns are performing against contract criteria to course-correct and maximize value-based revenue.
4. Enable Care Teams With Practical Tools and Processes
Operational success in value-based care depends on adoption at the front line. Care teams benefit from tools that support decision-making, reduce administrative burden, and align daily work with performance goals.
Action step: Engage clinicians, care coordinators, and operational leaders in solution design to ensure tools and workflows support care delivery rather than disrupt it.
5. Establish Continuous Performance Improvement Cycles
Organizations that treat value-based care as an ongoing operational discipline tend to improve faster over time. Regular performance reviews help teams understand drivers of variation and refine care operations throughout the year.
Action step: Implement recurring performance review cycles that connect analytics insights to operational adjustments and care model refinements.
Implications for 2026 Value-Based Care Planning
As organizations plan for 2026, the focus is shifting toward strengthening care operations as a foundation for financial and quality performance. This includes investing in analytics infrastructure, refining care delivery workflows, and improving coordination across clinical and operational teams.
Organizations that align strategy, care operations, and performance management are better positioned to manage risk, improve patient outcomes, and sustain results across value-based payment models.
How Tegria Supports Value-Based Care Operations
Tegria partners with provider organizations to operationalize value-based care strategies through the implementation of supporting technical functionality and the introduction and adoption of integrated care models. By aligning data, processes, and people, Tegria supports sustainable improvement in value-based care performance.
Ready to advance VBC performance?
Insight
Topics That Sparked Your Interest in 2025
As we close out 2025, we’re looking back at the ideas, questions, and innovations that resonated most with healthcare leaders this year. Across conferences, client conversations, and the insights we shared, a few themes consistently rose to the top, like navigating value-based care, establishing strong governance, modernizing data and analytics, and leveraging AI responsibly to support clinical and operational teams.
Based on what you viewed most, here’s a look at Tegria’s most-read content from 2025.
Navigating the CMS Shift to Value-Based Care: Are You Prepared To Succeed?
As CMS accelerates the shift toward value-based care, healthcare organizations increase focus on quality and cost-effectiveness of care. The shift means healthcare organizations must rethink their care model designs, data systems, and financial strategies as they transition to value-based care. Assessing readiness, investing in analytics and technology, and fostering a culture of collaboration can help position your organization for success.
Overcoming Capacity Management Challenges in Patient Access
Tegria’s CHIME survey found that capacity management remains a top barrier to patient access, with nearly all healthcare leaders citing it as a major challenge. Limited clinician availability, staff shortages, and inefficient scheduling systems hinder organizations’ ability to meet patient demand. Aligning technology with operational strategies, along with investing in interoperability and workforce training, can improve operational efficiency and access. Other strategies to enhance capacity management include standardizing referral management, using analytics to forecast patient demand, and promoting cross-team collaboration.
Navigating CMS-0057: What Providers Need To Know
While more attention has focused on payer responsibilities, healthcare providers also face significant challenges in aligning with the CMS-0057 Final Rule’s technical and operational demands. Although payers are regulated differently, provider compliance still demands technical and workflow changes to support seamless integration with payer systems. Key challenges include technical integration, workflow disruption, cybersecurity risks, financial strain, and navigating regulatory uncertainty. However, provider organizations that modernize infrastructure, invest in training, and collaborate with payers can turn compliance into an opportunity to improve care coordination, efficiency, and patient engagement.
Training for Tough Conversations: How Agentic AI Supports Healthcare Providers
Most clinicians receive minimal training in formal communication and how to navigate emotionally charged conversations. To address this gap, Tegria, Providence, and the Institute for Human Caring are collaborating to develop an emotionally responsive training tool that stimulates realistic, high-stakes conversations between patients and providers. This scalable, on-demand training approach aims to replicate the benefits of traditional actor-based roleplay. While many AI tools in healthcare are built to optimize workflows or streamline operations, this project highlights a different use case: supporting the human side of care.
Your Guide to Building a Proactive Healthcare Data Strategy
As value-based care and population health reshape the industry, organizations need real-time, trustworthy data to succeed. Building your data strategy rests on four foundational pillars: strategic alignment, data governance, scalable architecture, and advanced analytics readiness. Your data strategy roadmap progresses through distinct phases. First, establish your foundation by assessing your current state and defining goals with measurable KPIs. Next, build your technical infrastructure through scalable architecture and a robust governance framework. Finally, continue to cultivate a data-driven culture and continuous improvement mindset to transform your data into a catalyst for growth.
Fixing a Costly Billing File Error To Deliver Major Monthly Savings
A large Midwestern payer partnered with Tegria to resolve a recurring billing file error that was causing significant revenue loss. Tegria analyzed historical billing detail file trends, identified the root cause, implemented a backend fix to correct the logic, and validated improvements through a comprehensive comparison of post-fix billing files. The impact of the fix was immediate and substantial. Monthly billing losses due to errors dropped nearly 87% and enabled the payer to recover $780,000 in historical lost revenue.
Dive deeper into real-world success stories, expert insights, and proven practices with Tegria’s case studies and thought leadership.
Insight
Tegria’s Biggest Event Takeaways From 2025
2025 was another dynamic year in healthcare, and Tegria took part in the industry’s important conversations. After all we learned in 2024, we knew that this year would bring new momentum, intensified pressures, and evolving priorities across providers and payers alike. In case you couldn’t attend every conference, forum, or exhibition, this post gathers our experts’ event takeaways from the front lines of healthcare at events such as HIMSS25, ViVE 2025, KLAS Patient Consumer & Innovation Summit, and more.
From rapid shifts in outpatient care models and the rise of generative AI across patient access to mounting financial constraints, our team captured not only what leaders are talking about today, but where the industry is headed. Dive in to explore the themes that will shape your strategy, your operations, and your roadmap for the year ahead.
ViVE 2025
This year’s ViVE conference raised an important question: Are we addressing healthcare’s fundamental misalignments or reinforcing them with AI? Tye Cook emphasized the importance of rethinking your operating model before introducing AI. Leaders who implement AI without first aligning their operations risk automating inefficiencies and even creating new challenges. While technology can boost efficiency and expand access, without proper alignment, even the most advanced tools will fall short of their potential.
HIMSS25
At HIMSS25, Tegria shared key findings from The Health Management Academy regarding patient access and experience. The session highlighted the importance of a streamlined, operations-forward approach to technology to achieve improvements in patient access. We also presented with St. Luke’s University Health Network, sharing our journey in building a cloud-based Azure data lakehouse. Another highlight was our Lunch and Learn, where attendees gained practical guidance on how to evaluate AI opportunities. Overall, there were a lot of great sessions on data and information, health equity, technology, governance, and public policy.
MUSE Inspire
Key themes from MUSE Inspire 2025 included AI, interoperability, population health and analytics, cybersecurity, and patient engagement. In addition to those themes, we had the opportunity to share about regulatory compliance and financial performance. We joined Ashley Hall from White River Health to present a collaborative approach to regulatory readiness. Later, we presented an outcomes-focused productivity approach that healthcare organizations can adopt to drive strategic decisions and long-term revenue cycle improvements.
HFMA Annual Conference
The conference centered on three main themes: driving financial and operational transformation, embracing innovation, and prioritizing people. It highlighted how leaders are looking for performance improvement strategies with measurable ROI. Static reports are no longer enough. Leaders want modern data visualization tools to help them focus on the right priorities and act quickly. AI also generated strong interest at the conference. However, with limited resources, leaders are cautious and expecting proven ROI before committing. Denials were also top of mind, with a strong interest in technologies that can help ease the burden on staff and improve results.
AHA Leadership Summit
The AHA Leadership Summit reinforced a central truth about what matters most in healthcare transformation: people. Key themes included partnership, investing in the employee experience, effective change management, patient access, and people-first transformation.
At the summit we heard, “People don’t resist change—they resist uncertainty.” Leaders who intentionally embed change management into every initiative can better equip their teams to thrive. While technology plays an important role, we find lasting impact comes from cultivating a strong culture, building trust, and leading with compassion.
KLAS Patient & Consumer Innovation Summit
A key message from the summit was that meaningful innovation starts with listening to patients and designing around their needs. Today, organizations are intentionally incorporating patient feedback into strategic decisions, which improves patient satisfaction, trust, and loyalty. AI, when used well, can support more personalized, understandable interactions. The summit also emphasized offering patient education in multiple, on-demand formats to empower patients to make more informed decisions. Insights from the KLAS Patient & Consumer Innovation Summit reflect a broader movement toward patient-centered digital transformation.
MEDITECH LIVE 25
MEDITECH LIVE 25 was MEDITECH’s highest-attended leadership summit to date. A major theme of the event was that modernization is no longer optional. Some vendors are winding down support for legacy platforms, so health systems cannot afford to stand still. Another theme was that AI is moving from concept to embedded strategy. Many sessions showcased how AI solutions embedded within Expanse are driving results. Upgrading to Expanse 2.2 further enables organizations to adopt the latest interoperability features and automation. Lastly, community and collaboration continue to drive progress. MEDITECH LIVE provided an opportunity for providers, technology partners, and service organizations to come together and reimagine care delivery.
HPA Fall Leadership Forum
From navigating regulatory changes to market pressures and trends, health plan leaders discussed a variety of pressing topics and challenges at the HPA Fall Leadership Forum. During our fireside chat with the Community Health Plan of Washington and Network Health, we discussed payer-provider collaboration, tools for sharing clinical data, and different Epic solutions. While payers are at varying stages of adoption, attendees found it valuable to learn how peers are navigating choices and balancing demands. All in all, the event provided a dynamic space for health plan leaders to engage in meaningful conversations and explore future-focused strategies.
CHIME25 Fall Forum
As we saw at other industry events, AI is increasingly being integrated into everyday operations. IT governance is becoming essential for safe AI deployment, data quality, and strategic alignment. It comes as no surprise that community and rural health systems continue to struggle to keep pace with modernization because of financial strain and overstretched IT teams. CHIME25 highlighted that, while organizations are progressing at different speeds, they face common challenges. Clear governance, practical AI strategies, strong security, and modernization are vital to success.
Thank you for following along with our 2025 event takeaways. We look forward to connecting with you as we continue advancing meaningful conversations in 2026.
Insight
Key Takeaways From CHIME25 Fall Forum
CHIME25 Fall Forum in San Antonio reinforced why this gathering remains one of healthcare’s most valuable spaces for honest conversation and peer learning. Tegria’s attendees, which included Jeff Webber, Managing Director of Enterprise Systems & Services, and Chad Skidmore, VP of Technology Services, spent the week immersed in discussions about modernization, governance, AI, and the realities facing health systems of all sizes.

Here are the themes that stood out.
AI Moving Into Everyday Operations
AI dominated the conference, but the discussions centered on real-world adoption rather than abstract possibilities. Health systems shared examples of ambient clinical tools now in routine use and highlighted fast-growing interest in operational AI aligned with financial and workforce challenges.
AI has very rapidly moved from hype to a range of practical and successful use cases. Ambient technology is already becoming common, and I heard several examples of AI supporting operations in both provider and payer environments.
CHAD SKIDMORE
Organizations are at very different stages, with some implementing AI at scale while others are piloting. Many are still drafting governance and policy frameworks. Community and rural organizations are generally adopting AI through features embedded within existing platforms, especially major EHRs, allowing progress within limited staffing and budgets.
The Growing Importance of Governance
IT governance surfaced as a central theme across multiple sessions. Leaders described an expanding set of responsibilities, with technology decisions now intertwined with financial planning, workforce strategy, clinical operations, and risk mitigation.
IT’s role in organizational governance continues to grow, extending far beyond traditional technology decisions. More leaders are being pulled into broader strategic planning because technology now shapes so much of the organization.
JEFF WEBBER
AI is accelerating this shift. Many organizations are building governance frameworks to ensure safe deployment, manage data quality, track outcomes, and align initiatives with enterprise strategy.
Cybersecurity: Progress With Ongoing Pressure
Cybersecurity remained a top concern. Leaders discussed the lasting impact of recent high-profile attacks, the rise in cyber insurance requirements, and the growing complexity of proposed regulations.
Chad noted that past fear-driven spending pulled resources away from modernization efforts and may increase again as standards tighten. Jeff observed that some of the most mature cybersecurity programs are now led by outside CSOs, often former banking and government security leaders who can bring rigorous practices into healthcare.
Community and Rural Health Struggling To Keep Pace
Sessions focused on community and rural health highlighted widening disparities in digital maturity. Financial strain limits modernization. IT teams are small and often stretched thin. Innovation is slowed not by lack of commitment, but by lack of time, resources, and exposure to peer best practices.
Community health organizations continue to struggle with financial pressures that affect every part of their operations. The result is a widening divide between community organizations and larger urban peers, especially when it comes to innovation and modernization.
CHAD SKIDMORE
People and Relationships Still Define CHIME
Despite the focus on complex technology, the most consistent theme was the power of personal connection. The Forum’s intimate environment encouraged honest dialogue, strong peer interaction, and meaningful relationship-building. The experience reinforced how meaningful it is for healthcare leaders to invest in long-term relationships, returning to shared spaces like CHIME to build trust, exchange ideas, and accelerate progress together.
Looking Ahead
CHIME25 made clear that while organizations are progressing at very different speeds, they share common challenges. Clear governance, practical AI strategies, sustainable security, and a renewed focus on equitable modernization are essential.
Looking to a new season and year, we’re reminded that progress in healthcare technology depends on people. Thoughtful leaders. Collaborative peers. Partners who listen and build solutions grounded in real-world experience. As the industry continues to navigate rapid change, CHIME’s annual forum remains a place where leaders can align on what matters most and move forward with renewed clarity and purpose.
Insight
Driving Sustainable Change in Healthcare: A Conversation With Tegria and KLAS Research
In a recent episode of the “AHA Associates Bringing Value Podcast,” the American Hospital Association sat down with Meg Johnson, director of Care Operations at Tegria, and Robbie Bullough, senior director of consulting at KLAS Research, to discuss why structured change management is a strategic imperative in healthcare transformation. Their conversation explored how healthcare leaders can move beyond implementation checklists to foster true adoption, build trust, and sustain results over time.


Below are key insights from the discussion.
Q: Why is it critical to build change management into transformation strategies from day one?
Meg Johnson:
If you had the chance to make transformation successful, wouldn’t you take it? Research shows that effective change management makes it seven times more likely you’ll achieve your intended outcomes and ROI. Too often, we start with a project plan but forget the change plan—the equivalent groundwork that prepares people to engage and sustain transformation. Without it, organizations risk delays, budget overruns, and even long-term “change fatigue.” You don’t get many chances at large-scale transformation, so it’s vital to start strong.
Robbie Bullough:
When change isn’t planned from the start, costs multiply later—extra training, rework, system redundancies, even staff turnover from burnout. These are invisible costs at first, but very real when they hit. Like maintaining your home appliances, the ROI of doing change management right is that things keep working smoothly.
Q: Who needs to be involved early on to make transformation successful?
Meg Johnson:
Transformation affects everyone differently, so success depends on alignment across all stakeholder groups. Executive sponsors are essential. They must stay visible and engaged throughout the process. But frontline and mid-level leaders also play a critical role. They help uncover resistance early and build support among staff. The most successful organizations bring diverse voices to the table, even from outside their immediate structure, to build broad coalitions of support.
Robbie Bullough:
Operations leaders must have a voice in design and decision-making. When people feel change is done with them instead of to them, adoption rates soar. If operations are left out, resistance builds, and you end up fixing problems that could have been prevented by including them from the beginning.
Q: How can organizations integrate change management into their overall business strategy, not just IT projects?
Robbie Bullough:
It starts with leadership alignment and continues with clear, transparent communication throughout every phase, from preparation through sustainment. Change management isn’t a one-time task; it’s like a liquid that should flow throughout the organization.
Meg Johnson:
One of the most practical steps any organization can take right now is to equip leaders to lead through change. Build the “change muscle” at all levels so leaders understand their roles, the tools available, and the shared language for talking about change. That foundation makes it easier to activate when new initiatives arise—technical or otherwise.
Q: How should organizations measure success beyond technical metrics?
Meg Johnson:
We start by defining what success looks like early: What percentage of adoption is realistic, how quickly to expect results, and what outcomes truly matter. Then we track awareness, engagement, and capability through surveys and feedback loops. These insights let us adapt our approach in real time, whether by strengthening sponsor visibility or refining communication.
Robbie Bullough:
The feedback loop is critical. It’s not enough to collect feedback—you have to act on it and show people how their input led to change. When employees see that their voices drive decisions, they’re more invested in sustaining success.
Q: What advice would you give healthcare leaders to ensure change is sustainable long after go-live?
Meg Johnson:
Shift away from a “project” mindset. Go-live is just one moment in a longer journey. Adoption happens over time, and it’s fueled by honest feedback, transparency, and celebrating progress. When people see how their work connects to better patient outcomes, that’s what keeps change alive.
Robbie Bullough:
Exactly. Sustainability means managing change through and beyond go-live. These principles apply not just to IT but to any organizational change—mergers, restructures, process redesigns, anything that affects people. If you follow a structured, human-centered framework, you’ll create lasting transformation.
Listen to the Full Conversation
To hear the complete interview with Meg Johnson and Robbie Bullough, click here.
Insight
Realizing the Value of AI Starts With Data Governance and Leadership Support
By Mark Leifer, Data and Analytics Manager
AI dominates healthcare conversations. Vendors are knocking. Leadership is pressured to act. Pilots are sprouting across the industry. EHR vendors like Epic, Meditech, and Oracle are rolling out exciting AI tools that are embedded directly into their platforms.
Whether your organization is adopting those EHR-native tools or building a custom solution, one thing is clear: Data governance is foundational.
Amid the AI buzz, many health systems remain stuck in the proof-of-concept phase, unable to scale or sustain results. Gartner reports that, by 2027, 60% of organizations will fail to achieve the full value of their AI initiatives due to poor data governance.
In my experience, this isn’t a technology failure. It’s because the organization isn’t ready, and leadership hasn’t made data governance a priority.
Without Governance, AI Can’t Deliver Results
Imagine your organization rolls out a shiny new AI tool for clinical decision support. The logic is sound. It integrates with the EHR and the demo wowed the C-suite. But six months in, utilization is low, analysts distrust the data, and compliance wants to know who approved it.
This isn’t hypothetical. In fact, it’s a common pattern. AI stalls not because the tech fails, but because data governance was never embedded in the foundation. Behind that missing foundation is a lack of executive sponsorship.
Governance Needs a Seat at the Leadership Table
If AI is going to succeed in healthcare, data governance can’t live in the shadows. It needs executive backing, visibility, and resources.
Once an organization sets clear, business-aligned goals for data and AI, the next most important success factor is strong executive sponsorship. Ideally, that sponsor is someone with a C-level title — like a CIO, CMIO, or chief data officer — who can connect the dots between business strategy and the operational work of governance.
Modern data governance should emphasize accountability, clear decision-making authority, cultural alignment, and measurable outcomes rather than focusing solely on control. Executive sponsors are critical to bridging those priorities across business and IT. Their role is not to manage the day-to-day, but to model support, prioritize funding, and align governance with organizational goals.
When leaders show up to governance councils, reference it in strategy discussions, and reward good data practices, the signal is clear: This matters.
Culture, Not Control, Is the Real Barrier
Governance must move from fixing data to enabling confident use of data across the enterprise, from “AI as a cool tool” to “AI as a governed system.” Developing a strong data culture happens through modeling, incentives, and stewardship that’s embedded into real workflows. Without that cultural groundwork, even well-designed AI tools will flounder. Teams won’t know who owns the data. Trust will be low. People won’t feel confident using the outputs. Worse, they may not feel safe raising concerns when something looks off.
Build a Coalition, Not a Silo
Executive sponsorship is step one. Step two is building a data governance coalition that spans departments. This coalition — ideally a formal data governance committee — should include IT, clinical leadership, compliance, operations, and analytics. Too often, these groups are working in silos. This structure ensures that governance is positioned as a value enabler and a risk mitigator for AI adoption, rather than bureaucracy.
When it comes to AI, the governance committee should help define approval processes, monitor model performance, and ask questions about transparency, bias, and explainability. But they should also help build buy-in, provide feedback loops, and support training across the organization.
Is Your Culture Ready for AI?
Here are four signs that it may not be:
- No one can clearly answer who owns governance for AI tools.
- A promising AI pilot was shelved due to unclear accountability or lack of trust.
- Data decisions are made in silos or based on influence, not strategy.
- Governance is viewed as red tape, not a strategic capability.
If these sound familiar, you have work to do; but these are fixable problems.
Three Practical Moves To Build Executive-Led Data Governance
If your organization wants better AI outcomes, here’s what I recommend:
- Appoint a C-level sponsor for governance and AI readiness. This person should connect governance to business strategy. Not manage the weeds, but advocate visibly and consistently.
- Stand up a formal data governance committee that includes stakeholders from across the organization. Give it real authority, diverse voices, and a regular meeting cadence.
- Make cultural change part of the plan. Train people, talk about successes, and share stories where good governance led to better outcomes. Help teams see data governance as something that supports their work, not slows it down.
Final Thought
AI won’t transform healthcare if we treat it like a series of disconnected tech pilots. It must be guided by strategy, grounded in governance, and shaped by people who understand the intersection of data, operations, and clinical care. That kind of alignment demands executive leadership, cultural change, and above all, trust. And trust begins with governance.
This article originally appeared in HIStalk.