Whitepaper
Your HEDIS Implementation: Insights and Strategies for Success
As more healthcare organizations shift to value-based care, the Healthcare Effectiveness Data and Information Set (HEDIS) is a key component of this shift. HEDIS is a tool that can help healthcare organizations by measuring performance across key areas of care and outcomes, including access and availability, effectiveness of care, and behavioral health. By prioritizing a structured HEDIS implementation, leaders can transform raw data into actionable insights that fuel long-term quality improvement across the entire patient journey.
According to the National Committee for Quality Assurance (NCQA), which is the organization that develops and maintains the HEDIS measures, over 90% of health plans in the United States use HEDIS to measure their performance on important healthcare quality measures.
As HEDIS evolves into a "digital-first" model, NCQA is transitioning toward more efficient data collection that leverages Electronic Clinical Data Systems (ECDS) to reduce administrative burden and provide more timely insights.
Implementing HEDIS can be a complex and challenging process. Healthcare organizations must be prepared to collect and report data accurately, understand and comply with HEDIS requirements, and use the insights gained from HEDIS to drive meaningful improvements in patient care.
MARK LEIFERSenior Managing Consultant, Data + Analytics
In this article, we will explore strategies for healthcare organizations to prepare for HEDIS implementation, focusing on the people, processes, and technology required for a speedy and successful rollout.
Why HEDIS?
The most important thing to address before beginning a HEDIS installation is understanding “Why HEDIS?” Implementing HEDIS should align with a strategic decision to pivot to a value-based care model. Healthcare organizations and payers, such as insurance companies and government programs like Medicare and Medicaid, often use HEDIS metrics as the basis for value-based contracts. This means that healthcare organizations must prioritize HEDIS measures and incorporate them into their quality improvement initiatives to succeed in the transition to value-based care. Furthermore, NCQA's move toward "HEDIS 3.0" focuses on making data more useful and actionable year-round, rather than just for annual reporting.
The following are areas where HEDIS can benefit a healthcare organization and provide an answer to “Why HEDIS?”:
- Quality Improvement: Healthcare organizations use HEDIS primarily as a tool for quality improvement. By implementing HEDIS measures, healthcare leaders can identify areas for improvement and work to improve the quality of care provided to patients.
- Provider Performance: HEDIS measures are also used in some cases to evaluate the performance of individual providers within a healthcare organization. Leadership can use this information to identify high-performing providers and provide targeted support and resources to providers who may need improvement.
- Benchmarking: Healthcare executives can use HEDIS measures to compare their organization’s performance to industry benchmarks. This can help identify areas where the organization may be falling behind or excelling and can inform strategic planning efforts.
- Regulatory Compliance: Many regulatory bodies require healthcare organizations to report HEDIS data. By implementing HEDIS measures, healthcare executives can ensure compliance with these requirements and avoid penalties or other consequences.
- Consumer Transparency: HEDIS measures can also provide transparency to consumers about the quality of care a healthcare organization provides. By sharing HEDIS data with patients and other stakeholders, healthcare executives can demonstrate their commitment to quality care and build trust with their community.
Key HEDIS Updates for 2026
- New Measures for MY 2026 – Respiratory Status Assessment (RSA) and Follow-Up After Emergency Department Visit for People With Multiple High-Risk Chronic Conditions (FMC)
- ECDS-Only Reporting Expansion – For Measurement Year (MY) 2026, Screening for Depression and Follow-Up Plan (SDS) has transitioned to ECDS-only reporting. This follows the previous shift of Childhood Immunization Status, Adolescent Immunization Status, and Cervical Cancer Screening to ECDS-only.
- Sexual Orientation and Gender Identity (SOGI) – NCQA continues to integrate SOGI data into various measures to better identify and address health disparities.
- Telehealth and In-Person Requirements – While many measures allow telehealth, some visits, such as Well-Child and Adolescent Well-Care Visits, continue to prioritize in-person data for specific components.
- Measure Retirements (MY 2026) – Ambulatory Care (AMB) and Inpatient Utilization—General Hospital/Acute Care (IPU) have been retired to make way for more modern, digital-friendly measures.
- Digital Transformation Goal – NCQA aims to have all HEDIS measures fully digital by 2030, shifting the focus from retrospective manual "chart chases" to automated, electronic data exchange.
Read more about current HEDIS updates from the National Committee for Quality Assurance.
Who Should Be Involved?
The success of your HEDIS initiative will depend on engaging a diverse group of people with a range of skills and expertise across your organization. This collaboration ensures that every stage of HEDIS reporting is backed by clinical accuracy and technical integrity, preventing the data gaps that often stall quality improvement goals. Here are some of the key resources and their roles:

Executive Stakeholders
Executive stakeholders are responsible for endorsement, support, communication, and strategic direction for the HEDIS implementation process. They play a critical role in securing buy-in from other leaders in the organization, allocating resources and funding, and setting priorities for the HEDIS implementation effort. To ensure that HEDIS will be successful, executive stakeholders should demonstrate commitment by:
- Attending HEDIS project meetings.
- Being available to the project team for questions and issue escalation/resolution.
- Committing to use and champion HEDIS data tools in their own work (once live).
- Collecting and sharing feedback from their direct reports and colleagues.
- Identifying obstacles to adoption and assisting in finding solutions.
Subject Matter Experts
This should be a person(s) with in-depth knowledge and expertise in HEDIS measures methodologies and who has knowledge of the payer contracts in scope for the HEDIS implementation. In addition, subject matter experts should be expected to:
- Assist in identifying HEDIS use cases.
- Be the primary validators of HEDIS data and measures.
- Participate in decision-making and validation for programs associated with the contracts they oversee. For example, if you participate in an MSSP ACO, the MSSP manager should be included as a subject matter expert.
External Resources
Individuals outside your healthcare system are just as critical as internal resources, including your payers and your electronic health record (EHR) vendor. Be sure to identify who these vendor resources are and confirm their commitment to the project, including:
- Primary Account Representative
- Technical Contact(s)
IT Team
Your internal IT team will be responsible for executing the vision and decisions made by the executive stakeholders and subject matter experts and will partner with your external resources.
Building Your HEDIS Project Team
These IT resources are required for a successful HEDIS install:
- A Population Health Analyst will lead the HEDIS build and should be certified in the vendor's HEDIS module.
- An ETL Administrator will load external data received from the payer(s).
- A BI Developer and/or Data Aggregation Analyst will validate external data and develop HEDIS analytic content for validation and workflow support.
- Cross-team support/resources (HIM, Ambulatory, Billing, Interfaces) are needed to address workflow questions and possibly support and build tasks.
Ultimately, a successful HEDIS implementation is about more than just checking boxes—it’s about building a culture of excellence. By mastering the nuances of HEDIS reporting, organizations can turn their performance data into a powerful engine for continuous quality improvement and better patient outcomes.
Defining Key Processes
How an organization chooses to implement HEDIS will be influenced by multiple factors—including their EHR vendor, payers, and internal resource availability—but there are four primary topics to address BEFORE starting a HEDIS implementation.
1. Do Your Homework
Before any build, executive stakeholders and subject matter experts need to make many key decisions, including:
- Distribution: Who will see HEDIS data (clinicians, directors, others)?
- Programs: Which payers and contracts will be in scope, and which measures and performance periods will be included? For a first-time install of HEDIS, it is recommended that no more than 12 measures be in the initial scope using at least two years of historical data from payer claims and eligibility data.
- Measure Calculation: Review payer contracts to determine how each measure is calculated and whether your EHR vendor can support the calculation method.
- Data Sources: Decide which data sources to use, including adjudicated claims data (primary source) and secondary sources such as pre-adjudicated claims, local EHR data, and external clinical data or patient self-reported data.
2. Define Your Patient Populations
To meaningfully use HEDIS measures to drive change, you must first know and define which populations should be in play. As part of HEDIS planning, work with your value-based care stakeholders to define which patient populations, as defined by your payer contracts, to include in your HEDIS implementation. Then, work with your payers to obtain this information in an electronic format compatible with your EHR.
3. Partner With Your Payers
Prior to your HEDIS implementation, reach out to your payers and inform them that you will be implementing HEDIS. Items to discuss should include:
- Resources: Identify payer resources that can satisfy the technical requirements, such as providing electronic data files.
- Payer Scorecards: Ensure you are receiving scorecards from your payers. Payers will use this data in measure validation, so it’s important to become familiar with them prior to starting HEDIS. These reports show your payer’s view of your HEDIS performance.
- Data Files: Confirm your payer will be able to develop the necessary eligibility and claims files required by your EHR vendor.
4. Operational Planning
It is best practice to know how HEDIS will be incorporated into users’ daily workflows before starting implementation. Consider how your organization will handle training, change management, and ongoing support, and include this in the implementation planning.
The final consideration involving a HEDIS implementation is around technology. By considering these technical aspects, you can facilitate a successful HEDIS implementation that enables accurate performance measurement and drives improvements in the quality of patient care.
Aligning Your Technology
Data Integration
- HEDIS implementation requires gathering data from various sources such as EHRs, claims systems, pharmacy systems, and other data repositories. Ensure your technology infrastructure supports seamless integration and data exchange between these systems. Specifically, ensure your systems can support Electronic Clinical Data Systems (ECDS), which allow for the integration of clinical data from EHRs, registries, and case management systems
Data Aggregation and Analytics
- Implement a robust data aggregation mechanism that can efficiently handle large volumes of data. It should allow for data transformation, normalization, and aggregation to generate the required HEDIS measures. Advanced analytics capabilities are essential to process and analyze the data effectively. The move toward digital HEDIS means technology must support year-round data availability rather than just an end-of-year reporting surge.
Dedicated Build Environment
- HEDIS implementations span multiple months. Therefore, having a dedicated and stable environment to conduct build, testing, and data validation is critical.
Best Practice
Your build environment should be connected to a non-production database environment that can handle data integration and aggregation without impacting daily operations.
Performance Measurement Tools
- Develop or adopt performance measurement tools that accurately calculate and report HEDIS measures. These tools should automate the calculation process, apply the appropriate algorithms, and generate results in the required format.
Data Security and Privacy
- Protect patient data by implementing robust security measures, encryption techniques, access controls, and compliance with privacy regulations like HIPAA. Ensure that the technology infrastructure is regularly audited for security vulnerabilities and stays up to date with evolving best practices.
Reporting and Visualization Tools
- Develop reports and visualizations of HEDIS performance results. These may include dashboards, scorecards, and other reporting interfaces that allow users to explore the data, track performance over time, and compare results across different measures and populations.
Data Governance and Quality
- Implement strong data governance practices to ensure the data’s accuracy, completeness, and reliability for HEDIS measures. Data validation rules, quality checks, and cleansing processes should be in place to maintain high-quality data.
Scalability and Performance
- Ensure that the technology infrastructure is scalable to handle increasing data volumes and can support the growing needs of HEDIS implementation. It should be capable of processing data efficiently, providing timely responses, and handling concurrent users.
Workflow Integration
- Integrate the HEDIS measures seamlessly into the existing clinical workflows and systems healthcare providers use. This integration will help streamline the measurement process, reduce manual effort, and enhance efficiency.
Compliance and Auditing
- Maintain compliance with HEDIS reporting requirements, and stay current with updates and changes to the measures. Organizations should follow the annual HEDIS cycle, which includes public comment in February and the release of final technical specifications in August. Conduct regular internal audits to verify the accuracy and integrity of the data and reporting processes.
Sample Project Timeline for HEDIS Implementation
After considering all the elements that go into a HEDIS implementation, a timeline can be estimated.
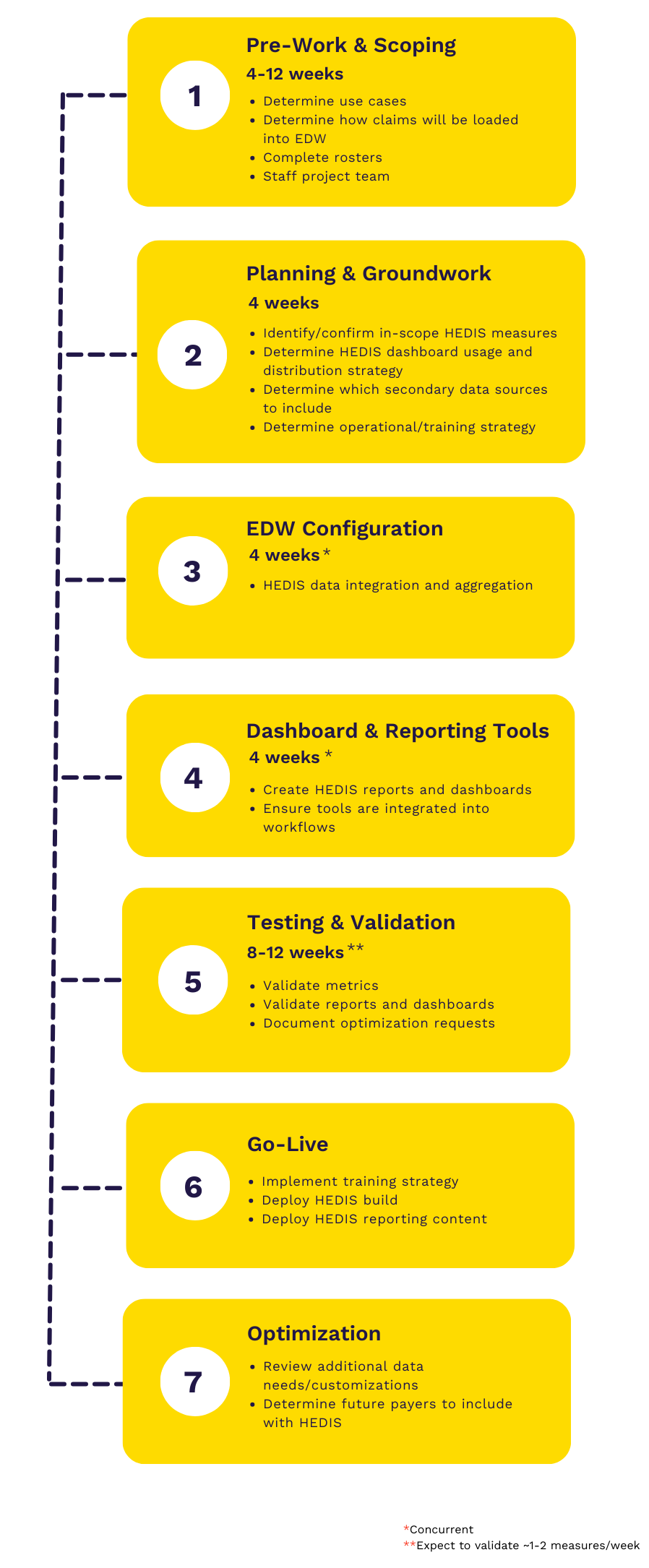
The following factors can influence the project timeline:
- Are you loading necessary claims information, patient eligibility information, and patient rosters?
- If yes: allow 3-4 months per payer line of business
- If no: allow 3-6 months of pre-work plus 3-4 months per payer line of business
- Variability based on responsiveness of payers, completeness of data files, and testing and validation of data files.
In addition, it is recommended that for a first-time install of HEDIS to take a phased approach. Complete one measure at a time: Build and test a single measure, including the downstream consequences of implementing that measure. Then, build and test the next measure, and so on. With this measured approach, when you run into issues, you know the source of the problem is the measure that you’re currently building and validating.
Conclusion
We have delved into the critical components of a HEDIS implementation and provided valuable insights for healthcare organizations seeking a seamless and efficient rollout. By prioritizing the people, processes, and technology involved, healthcare organizations can confidently navigate the complexities of HEDIS and pave the way for improved patient outcomes and quality care. With the right strategies, organizations can ensure a speedy and successful implementation, positioning themselves as leaders in the ever-evolving healthcare landscape toward value-based care.
At Tegria, we stand ready to support organizations in their HEDIS journey, offering tailored solutions and expertise to drive excellence and achievement. Together, let us embrace the power of HEDIS and unlock a future of optimized healthcare.