Article
Opening the Digital Front Door To Drive Patient Satisfaction
Approaching a digital front-door strategy with humans in mind can help healthcare organizations improve patient access.
Approximately 70% of patients are willing to switch healthcare providers for more convenient scheduling and better digital tools. The subtext for healthcare organizations: The industry needs to step up its game.
Healthcare organizations (HCOs) are struggling to deliver the experiences that patients want. Creating a frictionless digital front door can help HCOs give patients the convenient, technology-enabled experience they want. By centering patient experiences, taking cues from more digitally advanced industries, and understanding the best design approach to maximize return on investment (ROI), HCOs can create a better front door to care.
The digital front door is a strategy that leverages technology that patients have already adopted to drive success and satisfaction by engaging patients through every major touchpoint of the healthcare journey.
Considering the consumers’ struggle
Subpar experiences are far too common in healthcare. In fact, many consumers expect slow, inefficient service. Achieving first-contact resolution remains significantly below the industry benchmark of 80%, which means a healthcare consumer cannot accomplish their needs in a single phone call.
Typically, patients must navigate a website with hundreds of phone numbers and service offerings. Upon calling those numbers, they may reach someone and be told that a provider cannot see them for multiple weeks, or they may not reach anyone at all.
Making appointments with providers is just the tip of the frustration iceberg. Patients typically become even more overwhelmed when trying to coordinate their overall care. Accessing the healthcare system remains challenging, and navigating it once inside can be even more confusing. This is not the experience anyone should have to expect or endure.
Exploring technology’s potential
Technology looms as the solution to this long-standing problem. According to a Harris study cited during the HIMSS presentation, three-quarters of Americans state that technology would be helpful when navigating transactions and interactions such as scheduling appointments, obtaining test results, asking medical questions, paying bills and establishing care with a new provider.

The good news is that three-quarters are recognizing the need to move forward, and many have started digital transformation journeys. Unfortunately, they haven’t come far enough. Most HCOs are still in the early “contemplating,” “preparing,” or “building” stages of digital maturity, while organizations in other industries are in the “emerging” and “leading” stages.
While existing technology can improve access to care, HCOs have not fully embraced these solutions. Many healthcare organizations still grapple with clinic-based phone rooms that often terminate voicemails. Online scheduling usage still lags behind phone-based appointments. Lost referrals from Point A to Point B continue to be an issue, resulting in delays and extra work. Consistent financial transparency and the ability to provide cost estimates at the time of service remain unresolved.
Learning from other industries
Patients, however, expect to get more satisfying front-door experiences in healthcare because they are already interacting digitally in other industries.
By analyzing other industries, HCOs might discover other potential technologies to leverage, such as machine learning, which is prolific in other sectors. Integrating machine learning into scheduling algorithms and incorporating this feature into electronic health records (EHRs) can significantly improve the accuracy of the scheduling process and boost satisfaction for both providers and patients.
Adopting the right approach
Many HCOs are stuck in a holding pattern as they struggle with flawed or incomplete execution of these tools. To successfully move forward on this journey, HCOs need to adopt a human-centered-design approach for their digital front door. With this approach, HCOs should leverage market research and commission studies to create profiles for patients, providers, and front-end users. Beginning with an assessment of existing patient-access technologies and processes can yield invaluable insights to guide future initiatives.
During this process, HCOs can identify key touchpoints where the patient experience can benefit from an infusion of technology, which communication mediums are ideal for patients, and which technologies and investments can accommodate a better patient experience.
Investing intelligently
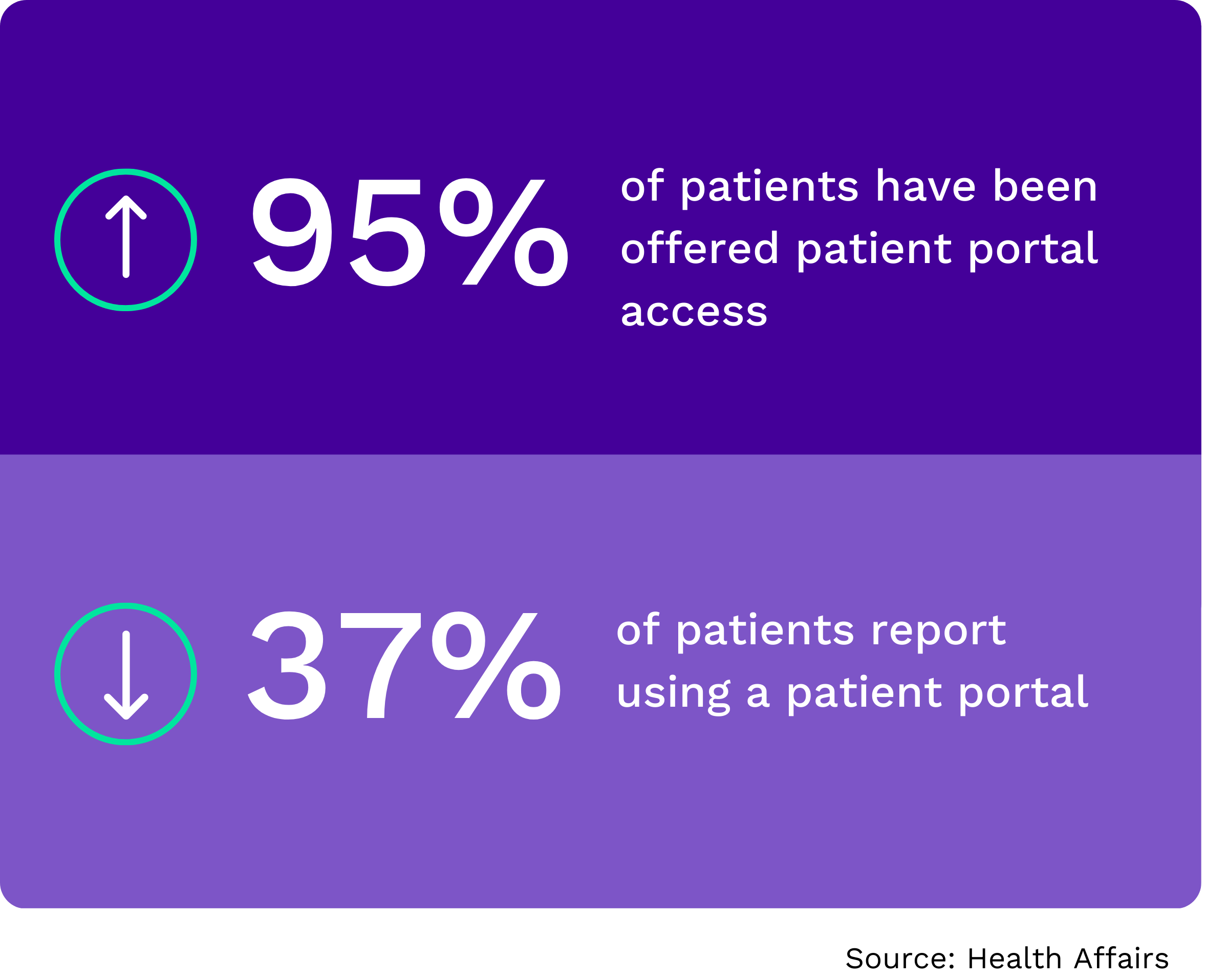
While healthcare offers numerous patient portals and online tools, their adoption rates remain disappointing. Just 40% of individuals nationwide accessed a patient portal in 2020, according to the Office of the National Coordinator for Health Information Technology.
The problem frequently boils down to design flaws. Patients often realize that, even if they complete forms online, they will have to go through these forms again in person. HCOs must evaluate their approach to achieve interoperability and seamless integration of consumer empowerment tools.
Finally, to continue providing superior patient access experiences, HCOs need to stay ahead of the curve. By envisioning the ideal state for patients, clinicians, and care teams, HCOs can help patients move beyond frustration to build fruitful, trusting relationships with their providers.