Resource
Payer Platform Services and Support
Improve integration, readiness, and outcomes.

Let’s leverage Payer Platform for smooth, seamless operations.
For a smooth and successful implementation experience, choose an Epic-experienced partner. With deep expertise across Epic modules, provider workflows, health plan operations, and software, Tegria can help payers anticipate, understand, and resolve technical and operational problems. Our team knows which questions to ask and how to collaborate with key stakeholders to meet your organization’s goals, budget, and timeline.
Tegria Capabilities
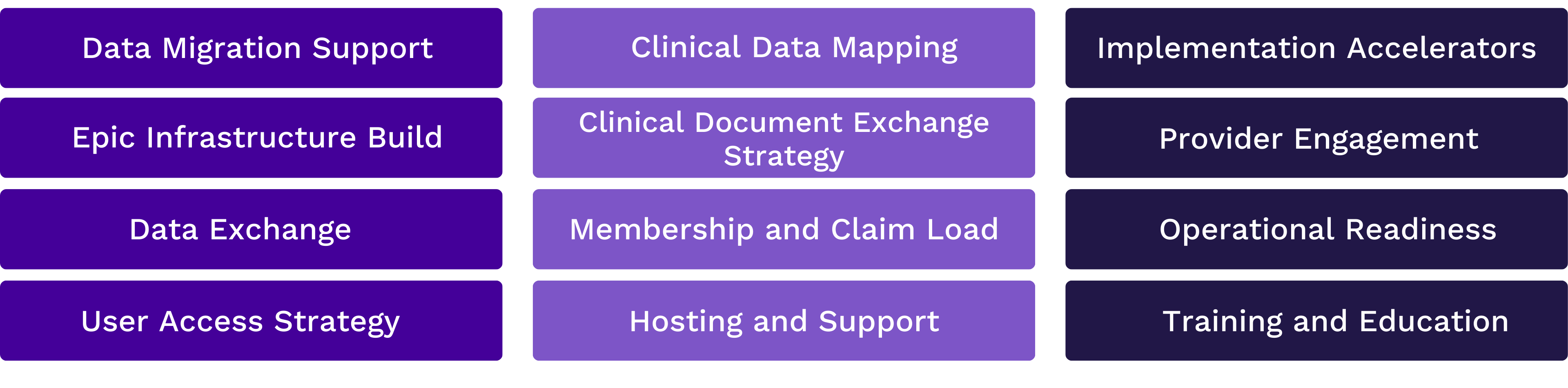
Tegria Can Help Payers Improve
Interoperability
Tegria’s integration analysts and data engineers work closely with your organization’s internal teams and third-party vendors to support data exchange across systems. Our consultants help payers share data with providers to view clinical claims and enrollment data in near real time, easing administrative burdens and addressing potential gaps in care.
Operational Readiness
Tegria also helps payers integrate Epic workflows into downstream systems to optimize your platform for peak performance. To maximize operational readiness, Tegria helps define functionality and system requirements, creates data mapping documentation, and supports change management throughout the project. Tegria’s use of implementation accelerators, including pre-developed templates, tools, and methodology, ensures a successful implementation at every phase.
Provider Relationships
Payer Platform helps health plans collaborate with providers and supports mutually beneficial exchange of data and administrative operations. Improving workflows supports provider enablement and builds better relationships between payers and providers. As Epic experts across provider and payer systems, our consultants support both entities to implement, optimize, and use Epic and define metrics to measure success.
ROI
Leveraging the value of an existing system helps control costs and improves data transparency between payers and providers. Tegria helps organizations assess data architecture, develop use case scenarios, and prepare for future needs while avoiding additional software purchases. Tegria helps identify incremental value at each stage of the Payer Platform implementation.
By leveraging Payer Platform, payers can reduce chart chasing, improve reporting and information sharing, and meet quality measures without extra administrative spending.